Our latest paper is a case report demonstrating substantial changes in HRV following concussion in a college football player. The full text can be accessed here. The main findings were:
1: The post-concussion HRV trend appeared similar to trends commonly associated with training fatigue. Therefore, staff should investigate the possibility of an unreported concussion when similar trends are observed in athletes.
2. Alterations in HRV persisted well beyond return to play clearance. This may have implications for clinical treatment and return to play considerations.
3. Since HRV demonstrated greater daily fluctuation post-concussion, isolated (i.e., single time-point) HRV recordings are likely inadequate for assessing persisting effects on the autonomic nervous system. Thus, near-daily HRV assessment may be required.
4. The convenient methodology used to monitor HRV (60-second finger-pulse plethysmography on a mobile application) can feasibly be implemented with an entire roster of athletes.
Abstract
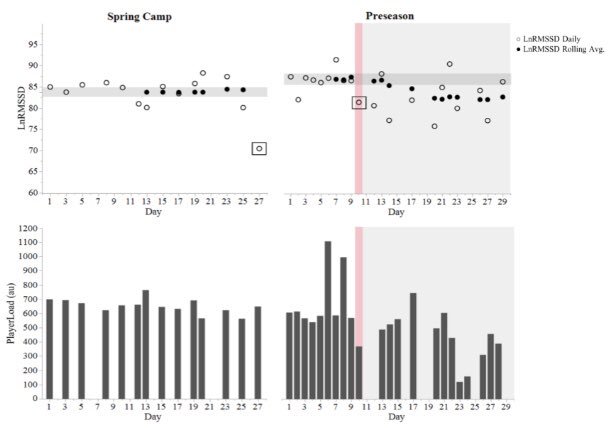
This case report demonstrates the effects of sport-related concussion (SRC) on heart rate variability (HRV) in an American college football player. Daily measures of resting, ultra-short natural logarithm of the root mean square of successive differences (LnRMSSD), subjective wellbeing, and Player Load were obtained each training day throughout a 4-week spring camp and 4 weeks of preseason training. SRC occurred within the first 2 weeks of the preseason. During spring camp and preseason pre-SRC, the athlete demonstrated minimal day-to-day fluctuations in LnRMSSD, which increased post-SRC (LnRMSSD coefficient of variation pre-SRC ≤ 3.1%, post-SRC = 5.8%). Moderate decrements in daily-averaged LnRMSSD were observed post-SRC relative to pre-SRC (Effect Size ± 90% Confidence Interval = −1.12 ± 0.80), and the 7-day rolling average fell below the smallest worthwhile change for the remainder of the preseason. LnRMSSD responses to SRC appeared similar to trends associated with stress and training fatigue. Therefore, performance and sports medicine staff should maintain regular communication regarding player injury and fatigue status so that HRV can be interpreted in the appropriate context. Detection and monitoring of autonomic dysregulation post-SRC may require near-daily assessment, as LnRMSSD showed greater daily fluctuations rather than chronic suppression following the head injury.