As the title implies, this is the third installment to a series I started several months ago that discusses the various factors that can help improve our HRV. The first two posts can be read by clicking on the respective links below.
How to increase HRV Part 1: Inflammation
How to increase HRV Part 2: Nutrition – Featuring contributions from my friend Marc Morris PhD(c)
I will first discuss (very briefly) some research and the key physiological adaptations that occur in response to aerobic exercise as it is these changes that ultimately affect the function of the autonomic nervous system (ANS). I will then provide some thoughts on how to include aerobic work into your training in effort to improve our overall health, recovery and capacity for training. Like always, I will include some anecdotal experience and a bit of theory. This article is primarily directed at strength athletes/individuals.
It’s important to clarify what exactly I’m referring to when I saw “aerobic exercise”. For the purpose of this article “aerobic exercise” is referring to some form of activity that maintains an elevated heart rate above resting conditions. This is a very broad and vague definition but for good reason. Depending on one’s current physical condition, aerobic work may be simply going for a walk, while in very fit individuals aerobic work may include longer distance running, swimming, cycling, etc. It can be tempo runs, circuit training, sled work, mobility drills or dancing if that’s your thing.
Aerobic Exercise as a Means to Increase HRV Among Various Populations
Children (age 6-11) who initially had low HRV scores saw significant increases in HRV after participating in a 12-month moderate exercise program (Nagai, 2004).
Elderly sedentary folks (men and women between 65-75 years old) saw an increase in HRV and cognitive test scores after 12 weeks of aerobic exercise (1hr/day, 3d/wk) compared to a group who performed only stretching (1hr/day, 3d/wk) of which saw a decrease in cognitive test scores (Albinet et al, 2010).
After 6 months of aerobic exercise training, both older (age 60-82) and younger men (age 24-32) showed an increase in HRV (Levy et al, 2004)
Gamelin et al (2007) put healthy young men (untrained, age 21) through 12 weeks of aerobic training followed by 8 weeks of detraining to determine its effect on HRV. An improvement in HRV was seen after the 12 weeks however HRV scores returned to pre-test levels after only 2 weeks of training cessation. “Twelve weeks of aerobic training are sufficient to achieve substantial changes in Heart Rate Variability; and only two weeks of detraining completely reverse these adaptations.”
I should mention that there are several studies that showed no improvements in HRV following exercise intervention. It appears that there is a threshold of exercise intensity required to augment vagally mediated HRV. Essentially, it’s important for heart rate to remain elevated beyond a certain level for a certain amount of time performed consistently over a certain time period for noticeable HRV changes to be seen. I realize that last sentence didn’t help anyone but I don’t believe this threshold level has been clearly established. My interpretation of the research that I’ve seen is that you simply need to be consistent and put more effort into it than a leisurely walk, although that may be a good start for some. Older people generally require longer exercise interventions as sympathetic activity increases with age.
Anecdotally, I can say that when I incorporate regular active recovery workouts (moderate aerobic intensity) my baseline HRV score is higher and I see quicker and higher spikes in HRV following an active recovery day. Furthermore, I almost always see decreasing baseline HRV trends when I do not include active recovery work. I can definitely see the corresponding relationship between HRV and aerobic work capacity. When my aerobic capacity is high my HRV is typically higher (baseline level). With consistent downward trends in HRV I’m typically detraining (due to illness, high stress, or anything that results in lack of training). Thus, at least in myself, when my aerobic capacity is higher, my HRV is typically higher.
* Note that this does not include acute changes in HRV but rather weekly/monthly trend changes.
Physiological Adaptations
Without trying to sound like an Ex. Phys text book I simply want to touch on some key adaptations that take place in response to aerobic exercise that influence ANS activity and therefore HRV changes. In response to aerobic exercise we will typically see that;
– Resting heart rate decreases
– Cardiac output increases
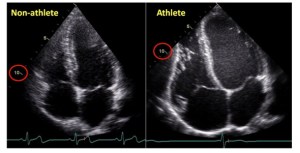
– Heart volume and size increases (Left Ventricle)
– Red blood cell size and count increases
– Capillary density increases
– Myoglobin increases
– Breathing rate decreases
– Blood pressure decreases
– Baroreflex sensitivity increases
– Renal-Adrenal function increases
– Parasympathetic tone increases
– Sympathetic tone decreases
*I used both the NSCA Essentials of Strength Training and Conditioning text and Primer on the Autonomic Nervous System Text for the above information.
I’m reluctant to say that all of the above directly affect HRV. The primary factors from the above list that impact HRV the most would be the changes in Sympathetic and Parasympathetic tone.
The ANS is responsible for responding to a stimulus/stressor and creating the necessary adaptations to allow us to resist the same stimulus/stressor in future incidences. Therefore, regardless of what type of athlete you are, improving your overall capacity for stress is beneficial. Our performance can be limited by our capacity for work. HRV score is a reflection of how much stress you can handle that day. Therefore we want to do what we can to position ourselves to better tolerate and adapt to our training.
Aerobic Work for Anaerobic Athletes
Let me be clear and state that I’m not advising powerlifters or throwers to go for a 1 hour run 3-4x/wk. However, in the interest of increasing workout volume/density and recovery, some aerobic capacity work can be helpful. Louie Simmons and Dave Tate have been preaching this for years. I recall plenty of articles where they discuss sled dragging, “feeder” workouts, etc. You can call this a “base” or “GPP”, “Anatomic Adaptation” or whatever you want. The bottom line is, we need to increase our body’s ability to handle training stress, recovery from it, then handle progressively more training again.
I understand that resistance training can elevate heart rate and maintain it over resting conditions. However, can you honestly tell me that you can go play a pick- game of basketball and not be completely winded after 5 mins? I used to not perform active recovery/work capacity workouts. If I did anything even somewhat strenuous for over 20 minutes that day my workout would be ruined. I’d purposely avoid physical activity so that I wouldn’t compromise my workout. Now that my work capacity is much higher I no longer have this issue.
Here are some thoughts on how to incorporate some aerobic capacity work into your training without negatively effecting strength progress;
– If it’s possible, take longer in your warm-ups. Here’s an example of a warm-up I do on Squat and DL days;
- 6 min aerobic exercise (incline treadmill, bike, skipping, etc), 5 min dynamic stretches, 5 min lower body mobility, 5 min “activation” type work for glutes and core (due to previous low back issues), 5 min upper body mobility (shoulders, t-spine) and external rotation work, some form of box jump or KB swing to finish. By the end of this I’m sweating and my joints feel great.
– Perform some type of activity on your off days. If you have terrible work capacity start off extremely easy with 10 mins of incline treadmill walking or the stationary bike. Over time work up to 20-30 mins. Generally I don’t exceed 40 minutes of work.
– Perform mobility circuits and kill two birds with one stone. Improve your mobility and aerobic capacity at the same time. Just keep your HR elevated.
– Perform low intensity sled work (various drags)
– Perform circuits of body weight exercise (Blast Strap/TRX stuff, single leg work, etc.)
– Complexes with BB’s, DB’s or KB’s.
Keep in mind that the goal is to facilitate recovery while at the same time gradually increasing work capacity. Therefore, do not perform 20 sets of hill sprints or maximal effort complexes on day 1 if you plan on moving any kind of decent weight that week. The goal is to;
- Maintain an elevated heart rate
- Enhance blood flow to sore muscles
What about intervals?
Yes, interval work can provide much of the benefits that aerobic exercise has to offer. However, intervals are much more stressful and taxing. Interval work can be better tolerated after a sufficient level of work capacity has been established. If you’re not concerned with strength levels than by all means proceed with intervals. However keep in mind that conditioning work with intervals is not necessarily facilitating recovery and will likely result in a lower HRV score the following day. Assess your situation and goals and make an appropriate decision.
If you progress your work capacity properly you shouldn’t see any negative effect on your strength levels. This isn’t about “concurrent” training were we want to build endurance and strength at the same time. It’s more about keeping strength the priority and gradually building work capacity at an intensity low enough that it doesn’t contribute to overall stress but rather facilitates recovery from it. This is how I prefer to do it.
Approaching this with athletes in a team setting is a different animal and I will hopefully share my thoughts on that another time as this article is already longer than I wanted it to be.
Summary:
– Aerobic exercise will typically increase HRV, better HRV results in more favourable responses to training
– Aerobic exercise can be anything that maintains an elevated HR
– Strength athletes can benefit from increased work capacity
– Progress from very low stress active recovery work to higher levels over time
– Use these workouts to facilitate recovery, improve mobility, enhance blood flow and maybe do the stuff you need to do that you can’t get to during your main lifts
If you have anything to add, refute, share, etc. I’d love to hear it. Comment below or email me andrew_flatt@hotmail.com.
I joined Twitter recently so we can interact there too @andrew_flatt.
References
Albinet, C. A., Boucard, G., Bouquet, C. A., & Audiffren, M. (2010). Increased heart rate variability and executive performance after aerobic training in the elderly. European Journal of Applied Physiology. 109(4):617-24
Gamelin, et al. (2007) Effect of training and detraining on HRV in healthy young men. International Journal of Sports Medicine, 28(7): 564-70
Levy, WC., et al. (2004) Effect of endurance exercise training on HRV at rest in healthy young and older men. American Journal of Cardiology, 82(10): 1236-41
Nagai, N., et al (2004) Moderate physical exercise increases cardiac autonomic nervous system activity in children with low heart rate variability. Journal of the International Society of Pediatric Neurosurgery, 20(4): 209-14